Through extensive research, the medical community has identified risk factors that you should understand to increase your chances of a heart-healthy life. Risk factors can be classified into those that cannot be changed; risk factors that can be treated or modified; and risk factors that can contribute but whose overall impact has not yet been determined.
Risk factors that cannot be changed include being male, age greater than 65, and heredity.
The leading cause of death in men is heart disease.
One study that examined the gender differences in heart disease concluded that, in general, males may be less adaptive physiologically, behaviorally, and emotionally in coping with stressful events. As a result, men’s risk for heart disease is greater. If these conclusions are accurate, then this may also mean that modification of this risk factor is possible with the development of better coping mechanisms to stress.
Age greater than 65 increases the risk for a heart attack because the heart and blood vessels become stiffer as we age. Remember the heart is a muscle that is responsible for pumping blood (and its nutrient elements) around the body via the blood vessels.
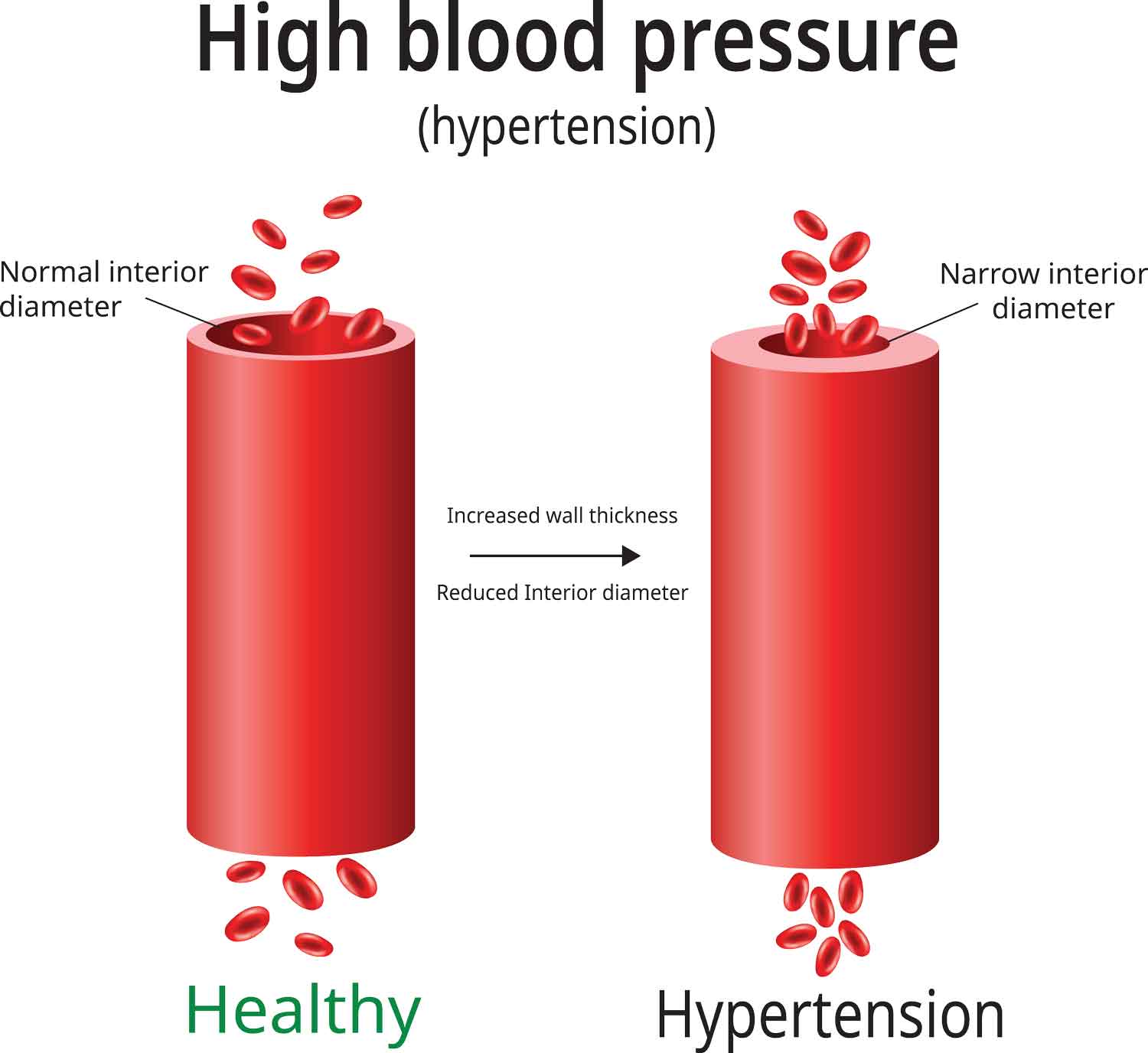
Blood vessels may be defined as an elastic tubular channel. But with age, the elasticity and flexibility of the channel decrease. If blood vessels become too stiff or narrowed, one of the effects is that the heart must work harder to distribute blood. One sign of developing stiff blood vessels is high blood pressure, or hypertension.
This explains why you should have your blood pressure checked periodically. Addressing any prolonged, abnormal increase can have positive effects on your heart health.
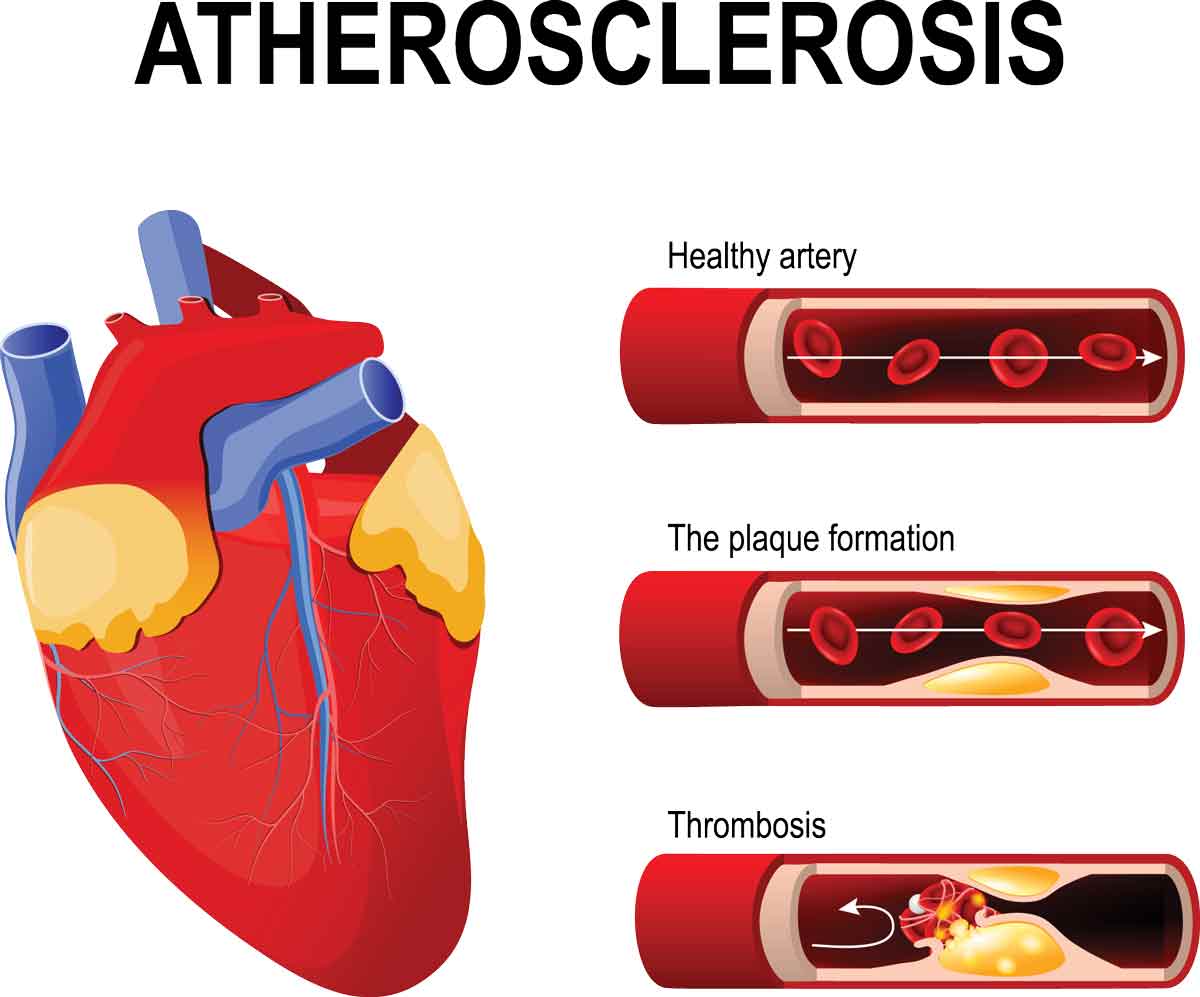
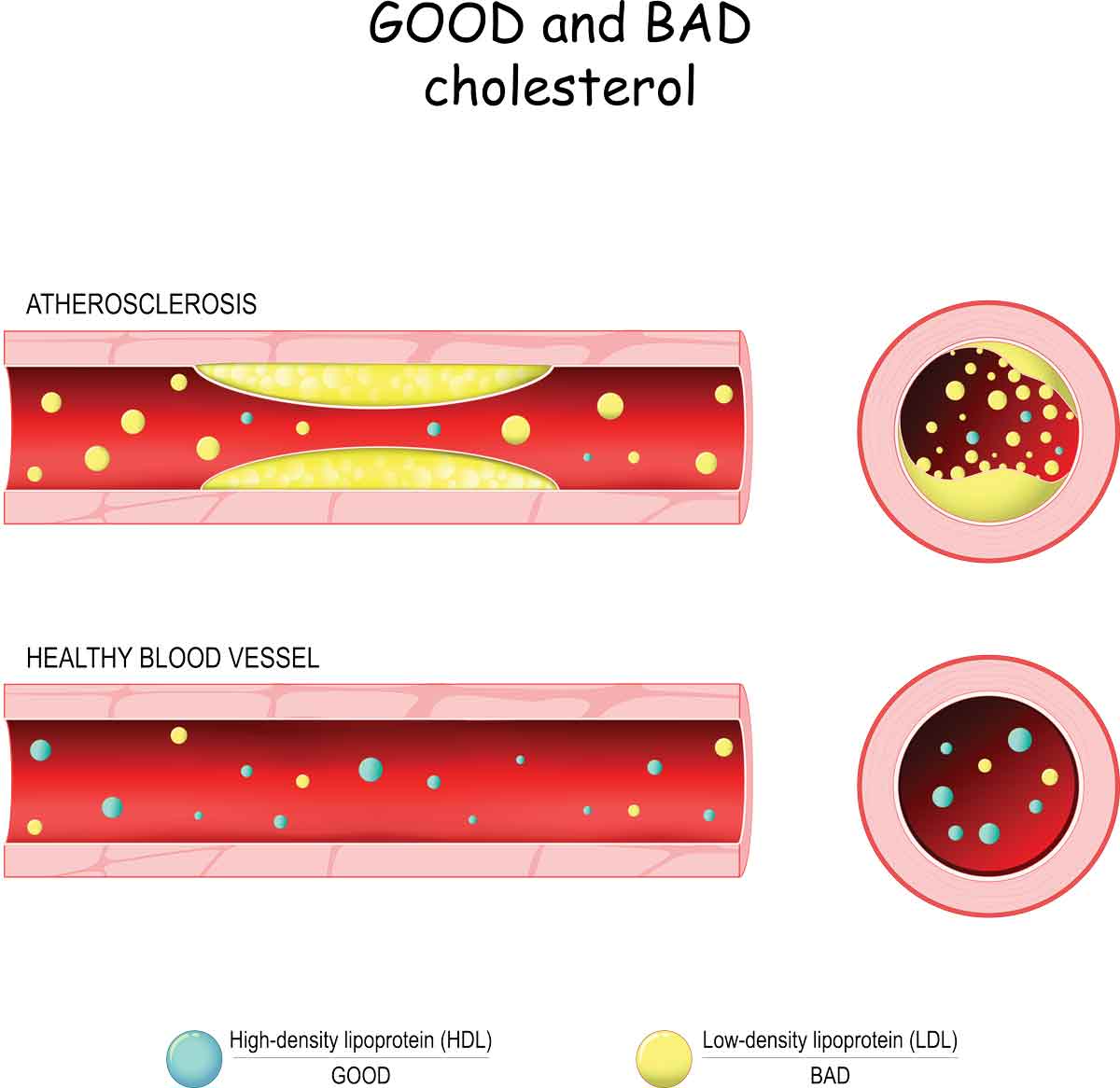
Another factor that can influence the stiffness of the blood vessels is the deposition of plaques inside the blood vessels. Plaques can be related to an individual’s cholesterol levels. Cholesterol is made naturally in the body, but certain foods we eat can also contribute to its presence in the body. If too much cholesterol is present, it can deposit in the blood vessels. In the heart itself, if the blood vessels to the heart become stiff, narrowed, or even blocked completely, nutrition to the heart can be limited or stopped, resulting in a heart attack.
The good news is that with careful monitoring of blood pressure and/or cholesterol, some age effects on heart health can be modified.
Heredity, or our genetics, is another non-modifiable risk factor for heart disease. The role of genetics by itself versus different cultural eating practices, diets, and lifestyles are difficult to separate. Nevertheless, certain ethnic groups have a higher risk for heart disease than others that can be genetically traced. For example, researchers have identified a genetic predisposition in African Americans whose line of ancestry originated in equatorial Africa. Specifically, those individuals from equatorial Africa had the ability to retain more salt from their diet. The researchers concluded that this allowed the body to conserve water in a hot climate, but it also predisposes one to retain salt and contributes to high blood pressure.
More research is needed to identify where interventions could be beneficial.
Modifiable risk factors include smoking, cholesterol, hypertension, diabetes, physical inactivity, and obesity.
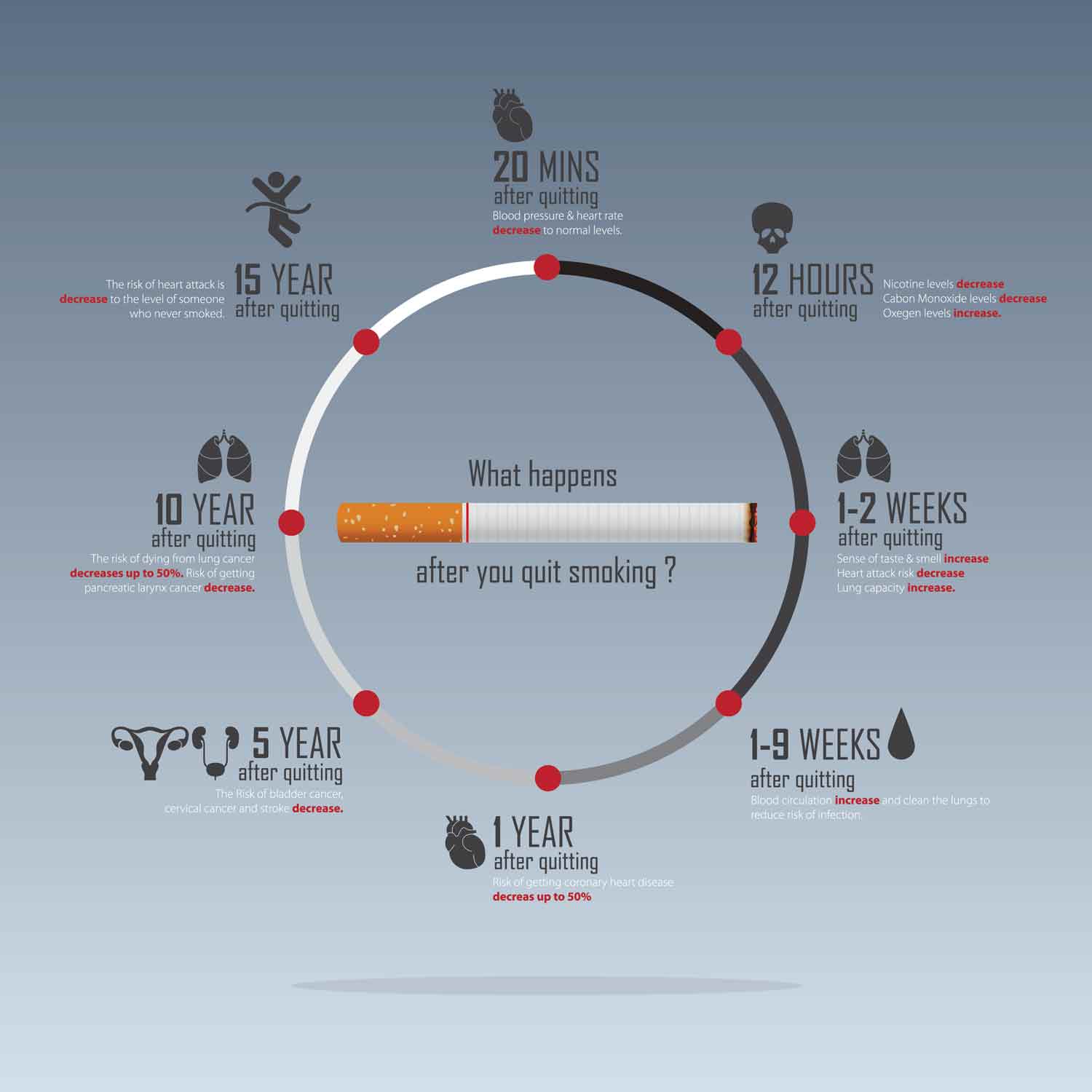
Smoking has been identified as a modifiable risk factor in heart disease. The chemicals in cigarette smoke have been found to damage the heart directly, blood vessels, and the elements in the blood itself. Interestingly, second-hand smoke has been shown to increase risks of coronary artery disease by 25-30% when compared to those not exposed. It is also important to note that e-cigarettes are not excluded from delivering harmful cardiovascular side effects. Quitting is the best safeguard to minimize tobacco’s negative effects on the heart.
As discussed above, cholesterol is a substance that our body uses to function normally. The problem comes when there is too much cholesterol. There are two types of cholesterol, LDL (bad) and HDL (good). Measurements of total cholesterol also include triglycerides. Too much of the bad kind of cholesterol (LDL), or not enough of the good kind of cholesterol (HDL), permits build-up in the blood vessels. Optimal recommended measurements are less than 200 for cholesterol, greater than 60 for HDL, less than 100 for LDL, and less than 100 for triglycerides.
The process whereby cholesterol and other substances are deposited in the blood vessels is also called atherosclerosis. Diet and, if necessary, medications prescribed from your doctor can help control cholesterol levels.
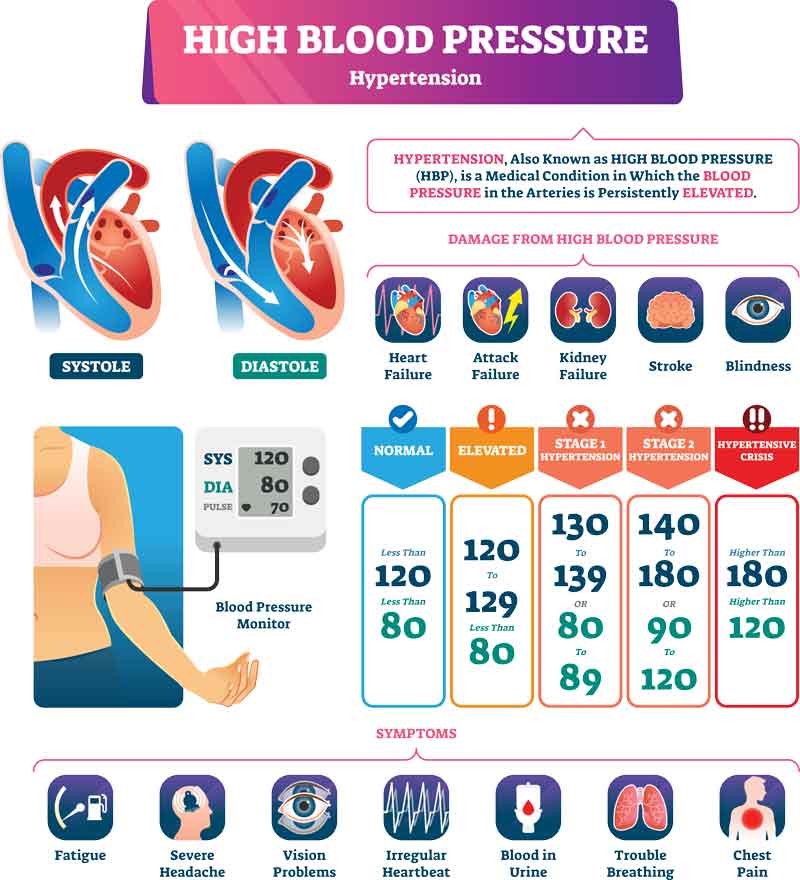
Hypertension is blood pressure that is too high. When your blood pressure is measured, it measures the pressures inside the arteries. There are two numbers that result: the systolic blood pressure; and the diastolic blood pressure. The systolic pressure refers to the pressure in the arteries when the heart muscle squeezes (or contracts). The diastolic pressure measures the pressure when the heart muscle is relaxing between contractions. https://medical-dictionary.thefreedictionary.com/blood+pressure Consistent measurements above 140 mm Hg systolic, or 90 mm Hg diastolic are considered too high. Treatments can be as simple as losing weight, decreasing sodium intake, exercise, limiting alcohol intake, and finding ways to relieve stress. Your medical provider can help determine what intervention is best for you.
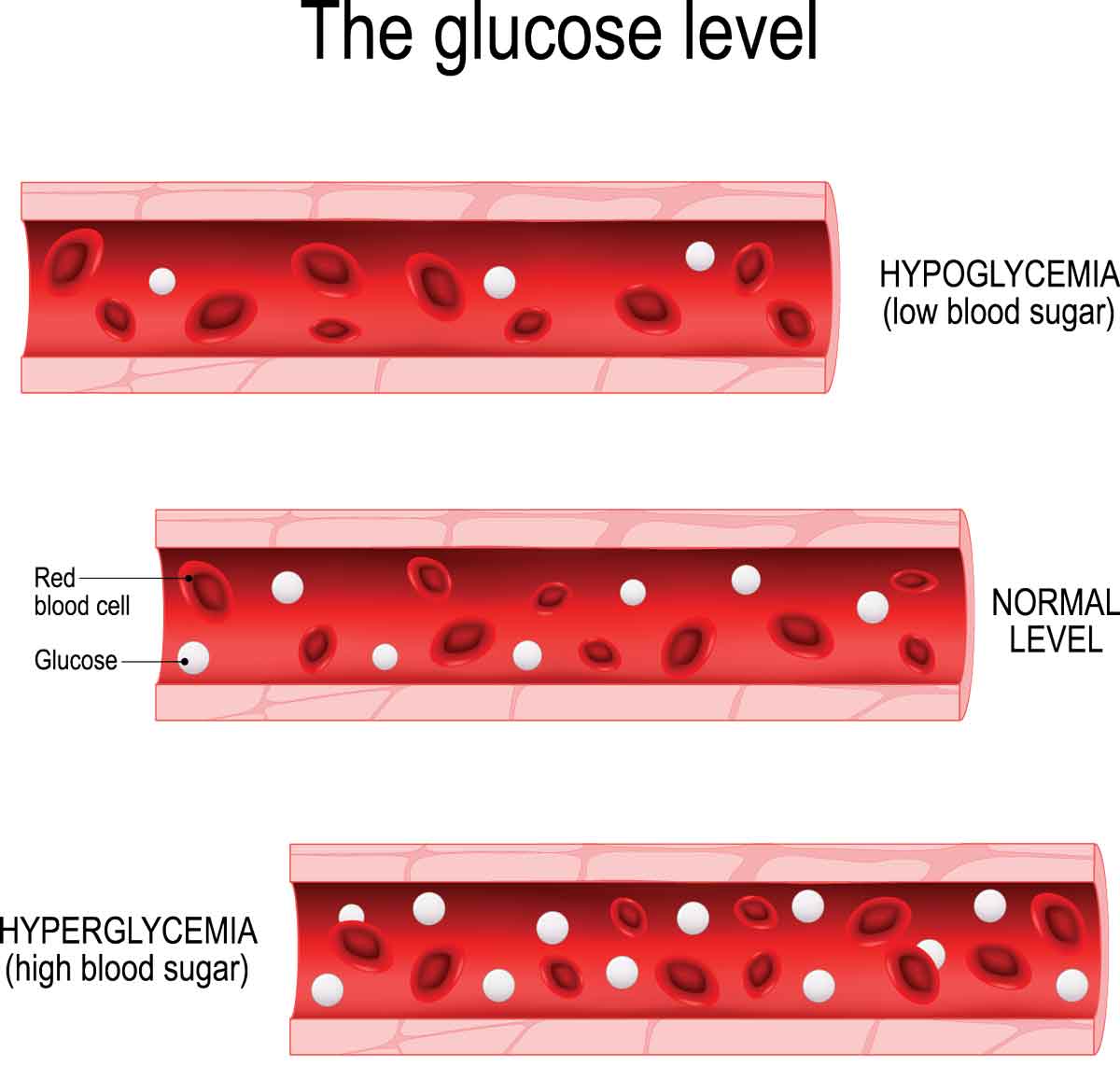
Diabetes (more specifically diabetes mellitus) is a condition where the body’s ability to metabolize sugar (glucose) is abnormal. This results in high levels of blood glucose.
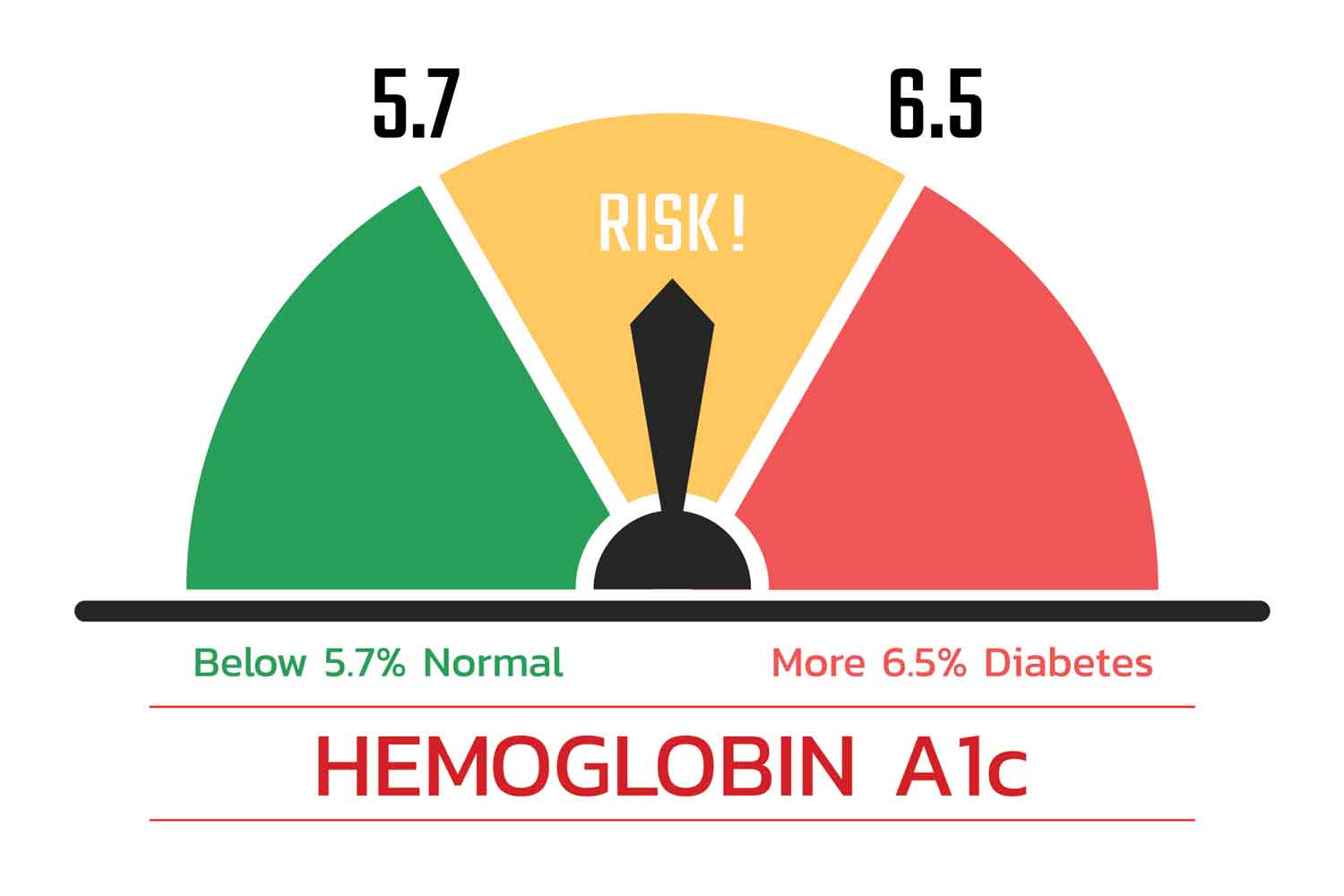
While the exact connection with heart disease is still being defined, studies show that individuals with diabetes are twice as likely to develop heart disease than individuals without. Controlling blood sugar levels through diet, exercise, and/or medications is thought to help address diabetes’ effects on the heart. For those with diabetes, knowing one’s Hemoglobin A1C, a laboratory blood test that measures how much sugar is on one’s red blood cells for the past approximately 3 months, helps dictate intervention. One’s goal should be to be below 5.7%.
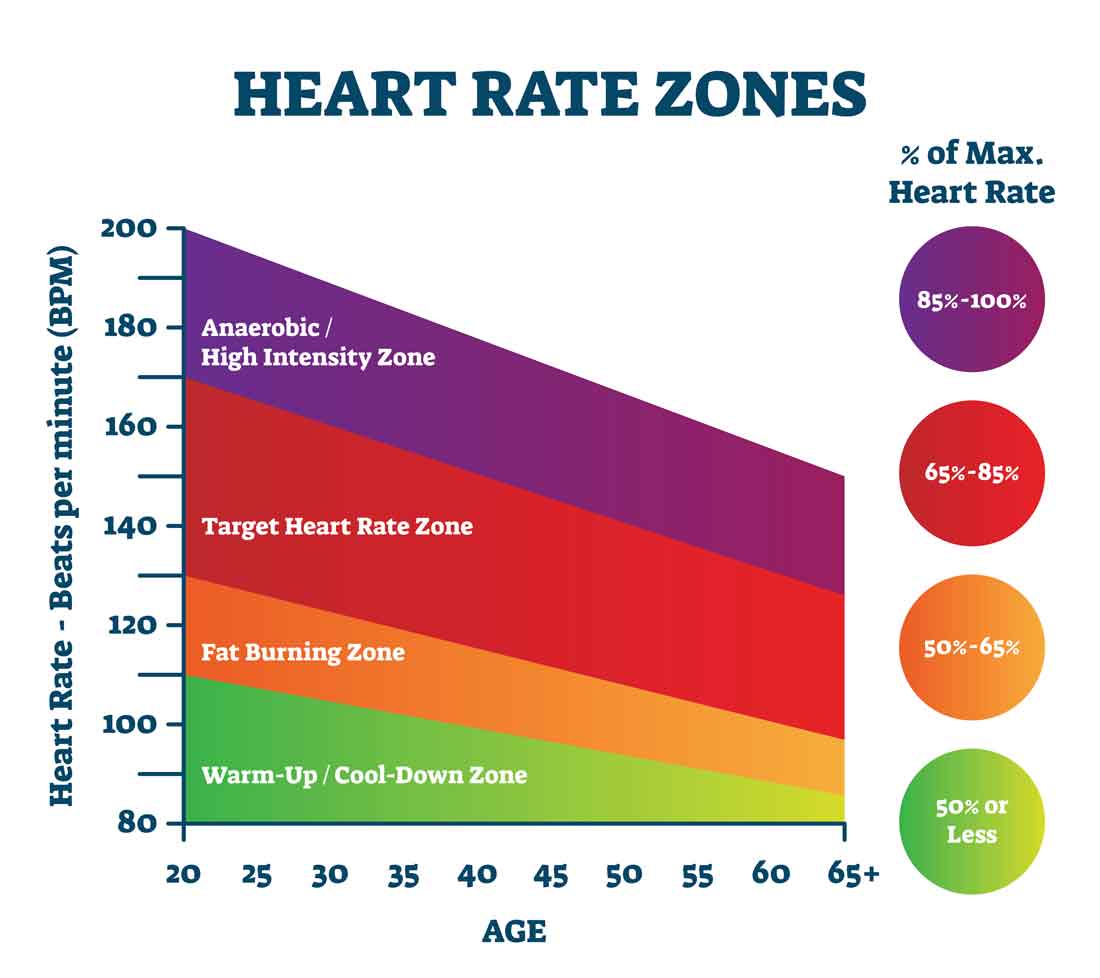
Proposed measurements of physical activity may be based on physical activity intensity, and target heart rate. Intensity of physical activity is divided into moderate and vigorous. Moderate intensity has been defined by the talk test. If during the activity you can talk, but cannot sing, then the activity is considered moderate. If during an activity you cannot say more than a few words without pausing for a breath, then that activity is considered vigorous.
Another way of measuring physical activity is by heart rate. For moderate activity, your heart rate should be approximately 65-85%% of your maximum heart rate. An estimate of your maximum heart rate is calculated by subtracting your age from 220. For vigorous activity, your target heart rate is 77-93% of your maximum heart rate. For adults, a goal of at least 150 minutes per week of moderately intense activity is recommended in addition to 2 days per week of activities that strengthen the muscles.
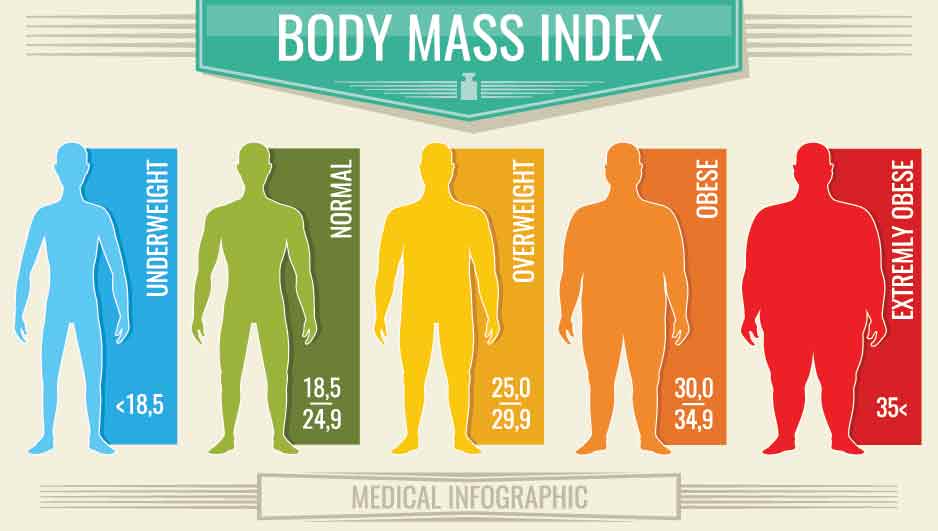
With respect to cholesterol, obesity can be an outward sign of the deposits that are occurring within the blood vessels. With respect to hypertension, greater blood pressure is required to deliver blood to a greater body mass–thus, the relation to blood pressure. And with respect to diabetes, obesity, as a state of overnutrition, causes the body’s cells to become resistant to metabolizing the glucose. Accordingly, addressing the risk factors of obesity and physical inactivity through diet, exercise, and medical intervention may also improve other risk factors related to cardiovascular disease.
Contributing factors include stress, alcohol, and diet/nutrition. These factors represent areas where more research is required to understand how each contributes to heart disease.
The body’s reaction to stress is to release adrenaline-which permits a fight or flight response. Among other things, the fight or flight response increases heart rate and blood pressure.
It is thought that long-term stress affects the cardiovascular system by creating an environment of long-term increases in heart rate and blood pressure. Inflammation has also been proposed as a by-product. Medical wisdom suggests that prescriptions are not the best way to address stress. Behavioral and emotional activities such as meditation, exercise, and other techniques to reduce stress are advised.
Alcohol as a contributor to heart disease is still being clarified. Moderate alcohol consumption (one drink/day for women and one-two drinks/day for men) has been said to lower the risk of heart disease by its effects on raising HDL, thinning one’s blood, and preventing damage from LDL cholesterol. The direct cause and effect relationship, however, has never been fully established. One must also be aware that any beneficial effects of imbibing alcohol were in the context of drinking in moderation. The American Heart Association states that drinking too much alcohol can raise triglycerides. Excessive alcohol can also lead to high blood pressure and cardiomyopathy (abnormal functioning of the heart muscle). In addition, empty calories from alcohol can contribute to obesity.
Diet and lifestyle have been identified as factors we have under our control that can affect heart health. Understanding the number of calories one takes in versus the amount burned can help regulate weight and obesity. Avoiding or limiting certain types of foods high in saturated fat, trans fat, sodium, and sweets can be favorable to the goals of heart health.
A number of factors contribute to our risks for developing cardiovascular disease. An understanding of those factors over which we can exert control helps optimize our heart health.
Dr. John, Esq. is both an attorney and a physician. Before obtaining his law degree, Dr. John Naranja practiced for approximately 12 years as an orthopedic surgeon.