COVID-19 has resulted in an explosion in the use of Personal Protective Equipment (PPE) to protect healthcare personnel, patients, and others. The CDC categorizes the capacity to respond to an increase in demand for PPE into three groups:
- conventional capacity relates to the implementation of conservative and administrative measures to lower the use or need for PPE
- contingency capacity relates to temporary measures to address the need for PPE
- crisis capacity relates to strategies that may not align with U.S. standards of care, but are considered as next best alternatives.
Measures from each group are intended to be executed sequentially. For example, on separate occasions, the Food and Drug Administration (FDA) has approved the use of filtering facepiece respirators that have been approved by the National Institute of Occupational Safety and Health (NIOSH), even after they have passed the manufacturers’ recommended shelf-life. The FDA is also involved with providing guidance regarding strategies to decontaminate facemasks and filtering facepiece respirators after use.
Another innovative approach to improving capacity is the use of 3D printing. Polytechnic University was one of the first to produce 3D printed facemasks for use in the care of COVID-19 infected patients. Each facemask takes approximately 3 hours to print on a standard 3D printer, but production can be more rapid with more workers assembling the units.
The 3D technology extends further to permit 3D printing of test swabs, Oxygen PEEP masks, ventilators, valves for oxygen masks, and hands-free door openers.
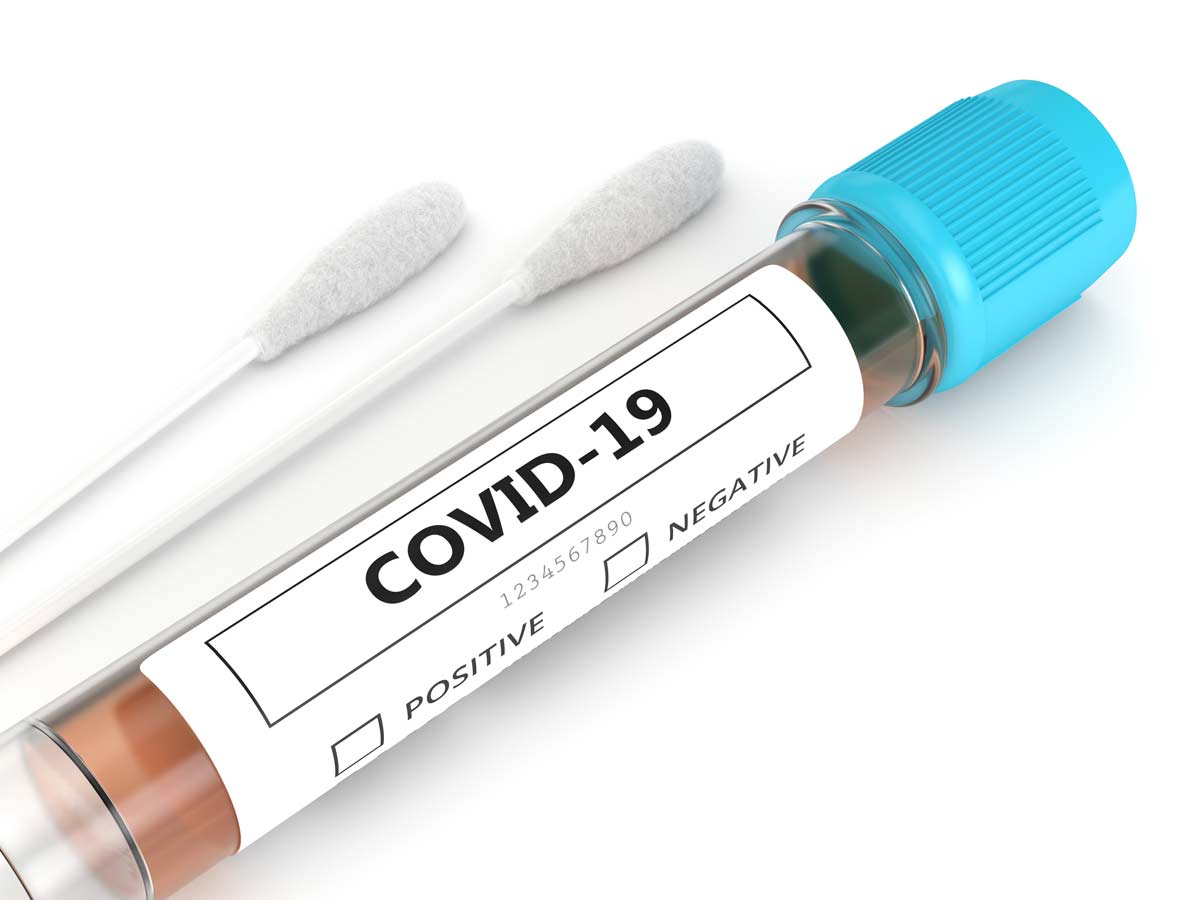
Test swabs refer to small flexible implements with a bristled end that is inserted in the nose to obtain a sample for testing. These items are in low stock around the world.
The Oxygen PEEP mask is a device that can reduce the time an infected COVID-19 patient would need to be on a ventilator. It works by introducing positive airway pressure into the lungs.
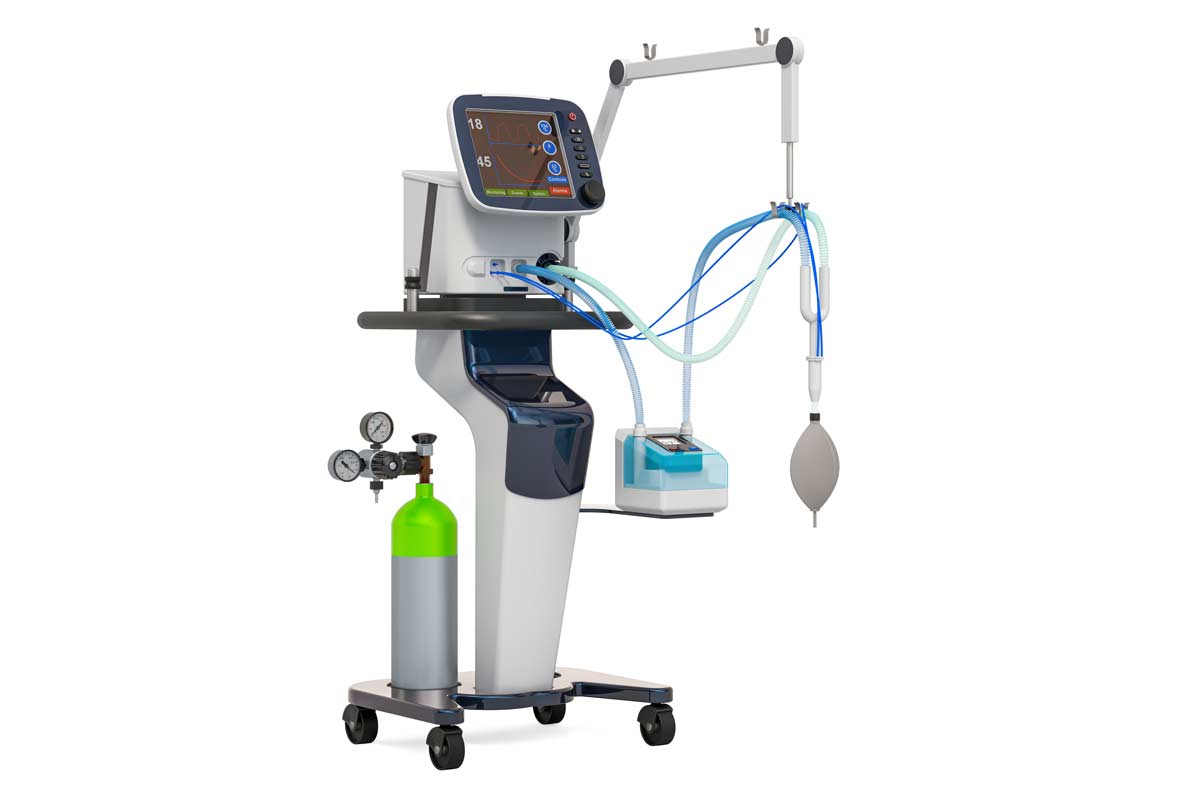
Ventilators are machines that perform breathing for those who are unable to breathe for themselves. The high demand for ventilators stems from severe COVID-19 infections that compromise the respiratory system.
Hands-free door openers are devices that allow individuals to open a door with their arms, reducing the risk of spreading the virus.
Valves for oxygen masks were one of the original applications for 3D printing technology. When a shortage of oxygen mask valves was identified in Italy, hospitals requested more valves from the manufacturer. When the manufacturer was unable to meet the demand, the hospitals made requests through the media. The call was answered by Christian Fracassi, founder of an Italian engineering startup. He reverse-engineered the valves and manufactured the valves with a 3D printer.
The National Institutes of Health has created an online file repository that collects 3D printer designs for COVID-19 related 3D devices. Medical testing and validation, however, have not been performed on all filings. Also, some products can only be made in facilities with a Qualities Management System present which includes an evaluation of sanitation conditions and only using skin approved materials.
For those who perform 3D printing, especially hobbyists, it is recommended that one consult with regulatory guidance as well as collaborate with FDA representatives.
Learn how lawyer Stan Helinski and his daughter started making respirators with 3D printers out of the house to help save patients suffering from Covid19. Learn how lawyer Stan Helinski and his daughter started making respirators with 3D printers out of the house to help save patients suffering from COVID-19. Click below to see the video:
Watch Episode 3 of The Hero’s Call..
Dr. John, Esq. is both an attorney and a physician. Before obtaining his law degree, Dr. John Naranja practiced for approximately 12 years as an orthopedic surgeon.