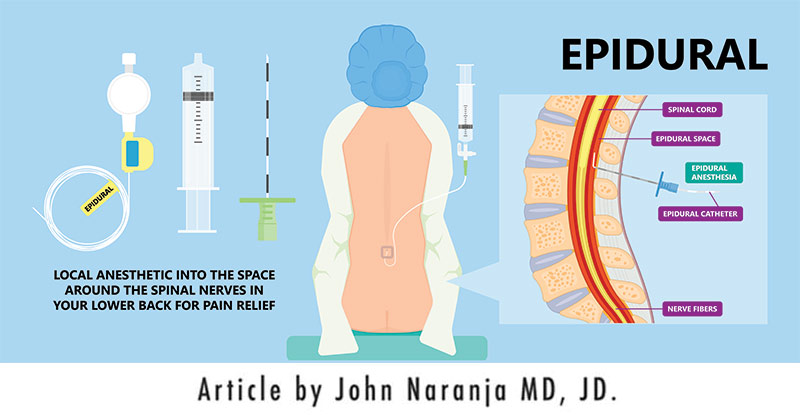
Epidural steroid injections are a common treatment for low back and neck pain that radiates into the leg(s) or arm(s) respectively. This article will discuss the anatomy involved in an epidural injection, what an epidural steroid injection is, why it is administered, results, and possible complications.
In a previous article, we discussed the coverings overlying the brain as it relates to head trauma. These coverings include the 3 meningeal layers: the pia mater; the arachnoid mater; and the dura mater.
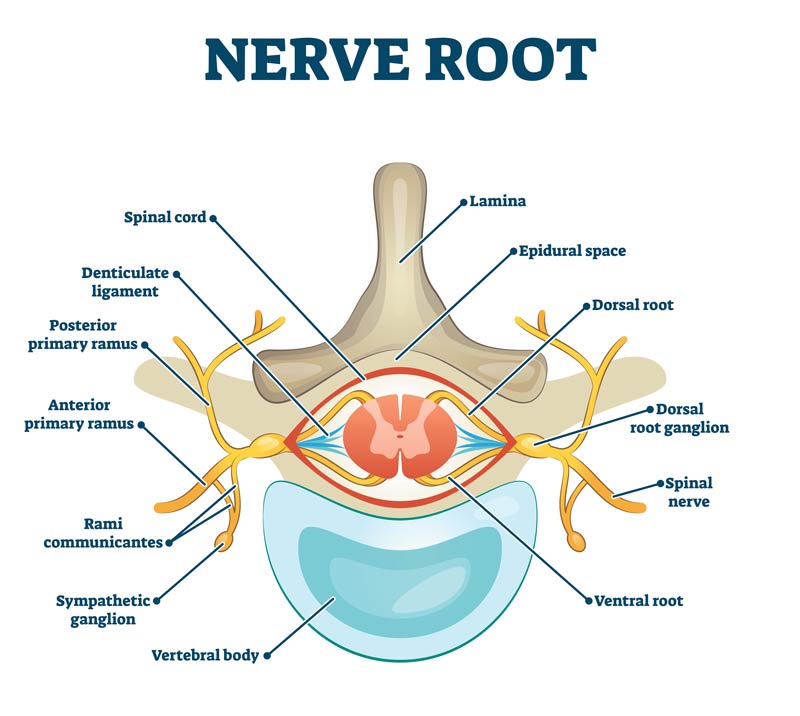
These same layers continue from the brain and extend to cover the spinal cord. The spinal cord itself is like a central electrical box that sends nerves to the different regions of the body. If something happens in the central electrical box that causes inflammation of a spinal nerve, a sensation of pain can be the result. Common causes of spinal nerve pain include a herniated disc, arthritic bone spurs, thickened or calcified ligaments, and/or anything that can cause inflammation or irritation around a nerve.
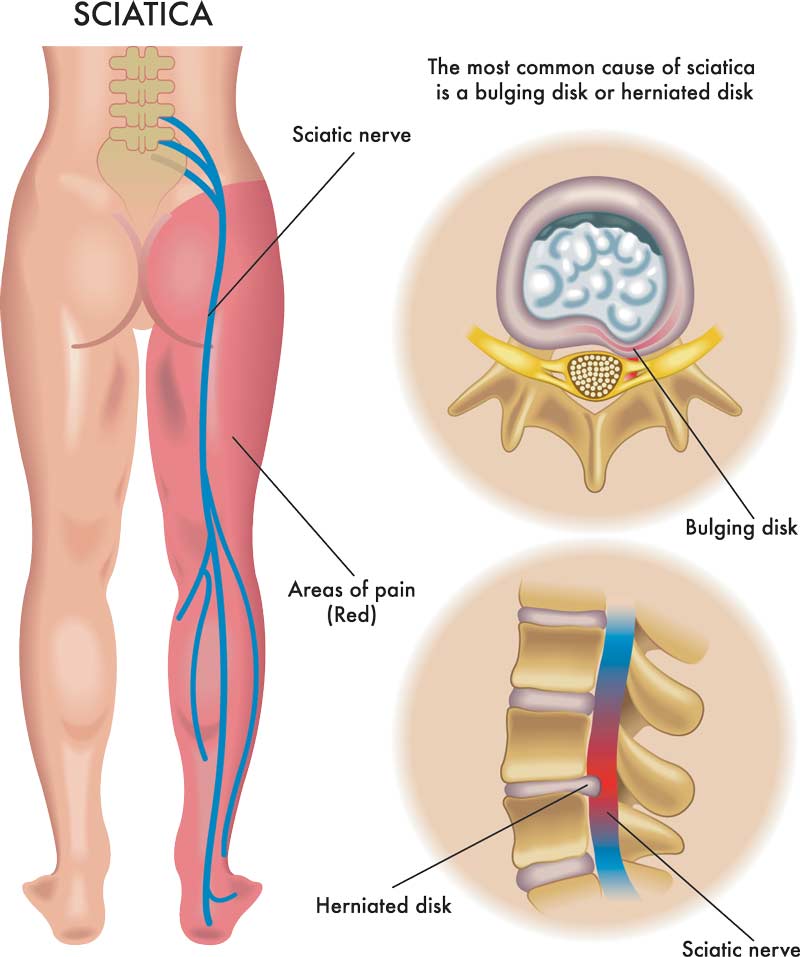
The following illustrations demonstrate two views of the spine where a herniated disc is putting pressure on the spinal nerve root.
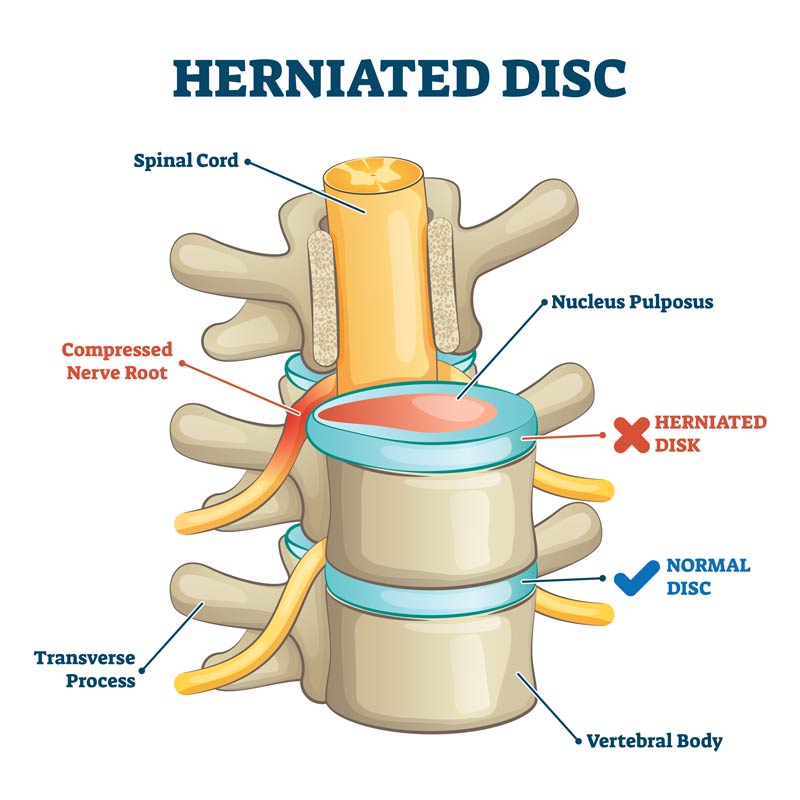
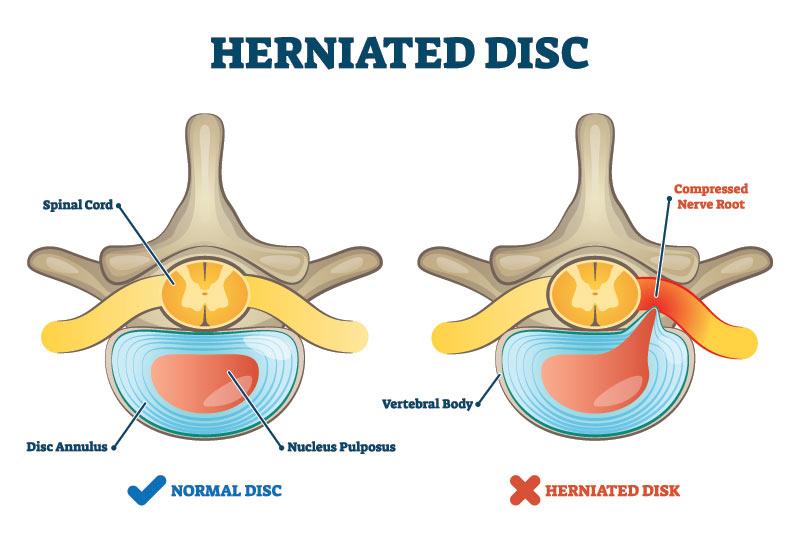
When more conservative measures like physical therapy, oral nonsteroidal anti-inflammatories, and traditional pain medications fail, or are only partially helpful, then an epidural steroid injection may be an option.
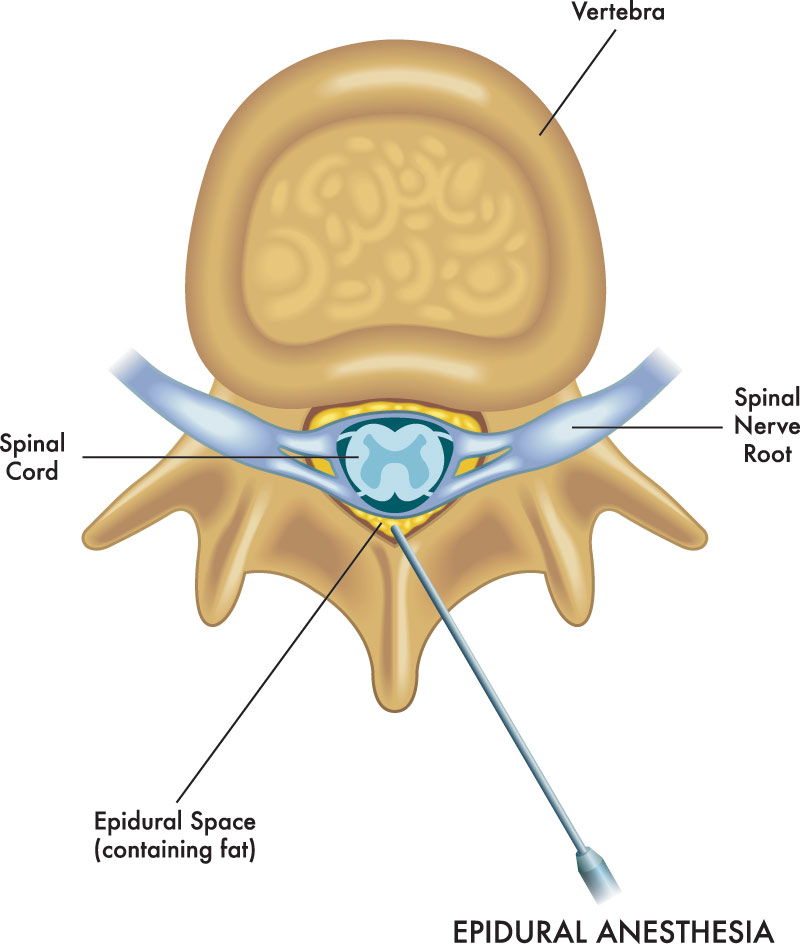
Treatment for nerve pain related to nerve impingement and/or inflammation with an epidural steroid injection relies on a working knowledge of the relationship between one specific meningeal covering over the spinal cord, specifically the dura mater. An epidural steroid injection is the placement of medicine, usually steroids, into the area outside of the dura mater.
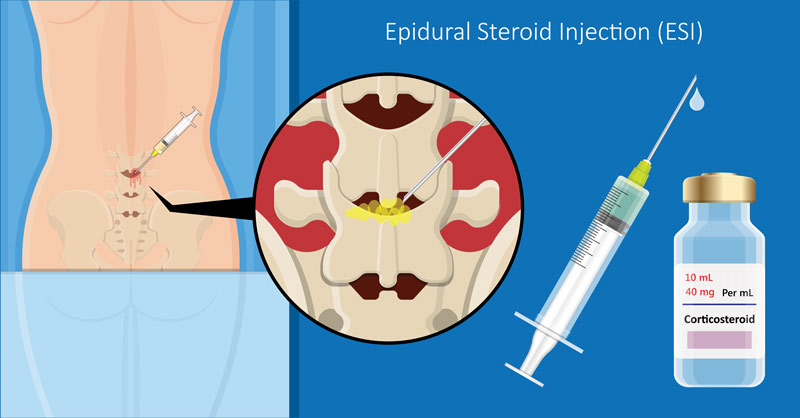
By administering the medicine via an injection, delivery is more direct and typically with a decreased dose, when compared with drug administration by mouth. Placement above the dura minimizes effects directly to the spinal cord. Administration in this manner can also help avoid side effects associated with higher doses of medicine. In particular, the purpose of the steroids is to reduce inflammation and fluid buildup around the spinal nerves that may be causing pain.
Epidural injections are usually administered in the area of an abnormality of the spine, as demonstrated by magnetic resonance imaging (MRI). For example, the injection can be administered in a specific area of the lumbar spine like L1, L2, L3, L4, or L5 depending on which nerve root is irritated.
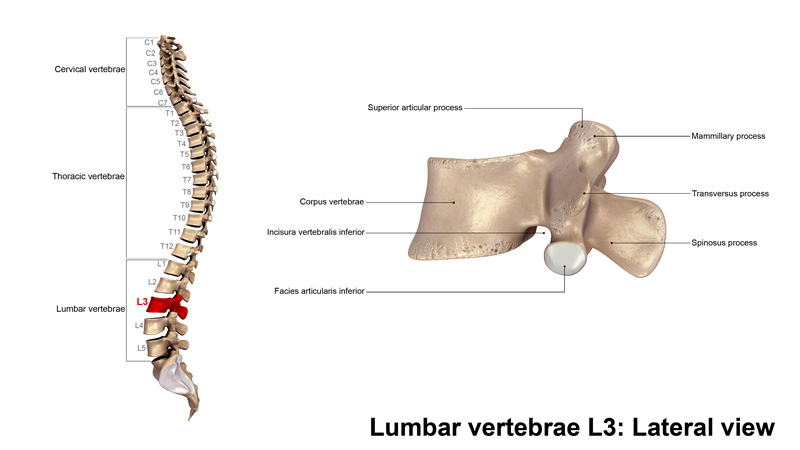
The illustration below is a side view of the different segments of vertebra with the L3 vertebrae highlighted.
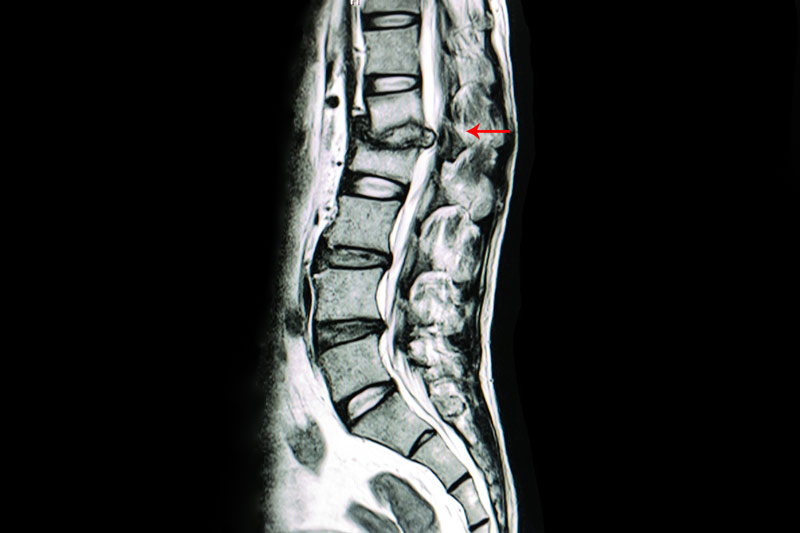
The physical examination and MRI are very helpful for identifying which herniated discs, bone spurs, and any narrowing where a spinal nerve could be pinched.
The type of symptoms that are relieved are usually radicular, meaning that symptoms that travel down an extremity in the same distribution as the nerve.
Radicular pain that travels down the leg has also been called sciatica.
Success rates with epidural injections vary, but in general, when administered for the proper diagnoses, the results can provide at least some temporary relief. One study publishes a success rate of 84%. It has also been demonstrated that higher benefits of epidural steroid injections were achieved in patients with a short duration of symptoms and a high percent of spinal canal compromise.
The injections may be repeated according to the recommendations of the provider.
Possible adverse effects and/or complications from an epidural injection include infection, blood sugar elevation in those with diabetes, bleeding, spinal cord injury, dural puncture. Less severe effects include skin depigmentation at the site of the injection, flushing, The most serious of these complications occur very rarely, but should be considered when undergoing the procedure.
Epidural steroid injections remain a viable alternative in the treatment of radicular symptoms related to inflammation of spinal nerves. Complications and adverse effects can be minimized with proper technique and highly experienced providers.
Dr. John, Esq. is both an attorney and a physician. Before obtaining his law degree, Dr. John Naranja practiced for approximately 12 years as an orthopedic surgeon.
